Title
Targeting neoantigens in multiple myeloma by TCR-transgenic T cells
Research Area
Hematology, Oncology, Immunotherapy
Project Summary
Adoptive cellular therapy (ACT) using TILs or TCR-transgenic (tg) T cells has shown durable responses across multiple cancers (1-3) and represents a promising treatment approach for multiple myeloma (MM), complementing CAR-T therapies (4). Traditional neoantigen-specific TCR (neoTCR) discovery relied on laborious functional assays (5, 6), while recent single-cell sequencing methods allow more sensitive, less biased identification (7-12). Optimization of neoTCR-based ACT requires detailed characterization of TCR function, T cell phenotype, and resistance to dysfunction (13, 14).
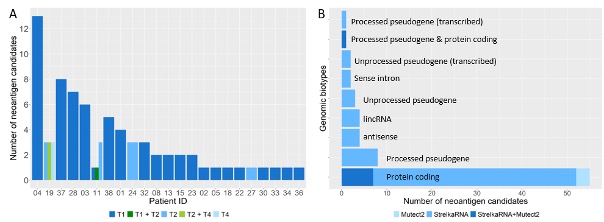
We refined our mass spectrometry (MS)-based neoantigen discovery pipeline to include RNA-derived neoantigens. Analysis of 32 patients from the MASTER cohort (15) using immunopeptidomics and whole exome/RNA sequencing revealed many neoantigen candidates originated from RNA variants – highlighting RNA’s underexplored role as a neoantigen source (16).
To test a more sensitive neoTCR discovery pipeline, we applied scRNA-seq and scTCR-seq to a previously characterized melanoma case (Mel15) where six neoTCRs targeting KIF2CP13L and SYTL4S363F had been identified (6, 17). This new approach confirmed known TCRs and revealed two additional KIF2CP13L-specific TCRs (KIF-sc1, KIF-sc2). Despite shared specificity, neoTCRs varied in clonotype frequency and activation strength. Functional assays of tg CD8+ T cells revealed a spectrum of activation from moderate to strong. In initial tumor challenge, all neoTCRs achieved comparable control. However, in a repeated antigen exposure xenograft model, moderately activating neoTCRs outperformed initially stronger ones (18).
These findings suggest a role for strong-activating TCRs in initial tumor debulking and for moderate-activating TCRs in long-term control. While activation profiles appeared TCR-intrinsic, we observed entity-specific differences. We expanded testing to MM by adapting cell lines (JJN3, U266B1, NCI-H929) via transduction of HLA, where necessary, transduction of tandem minigenes and peptide-pulsing for expression of KIF2CP13L and SYTL4S363F epitopes.
Activation patterns mirrored previous findings (18). Given CAR-T benefit from CD4+ help (19), we assessed neoTCR-tg CD4+ T cells. Although MHC-I-restricted, neoTCR-tg CD4+ cells showed activation after neoantigen-specific stimulation. Notably, moderately activating TCRs (KIF-P1, KIF-sc2) showed strong CD4+ activity, suggesting partial CD8-independence – confirmed using Jurkat models. These findings further expand the neoTCR activation and functionality landscape.
Temporal analysis in MM co-cultures revealed a peak in activation at 12 h. Strongly activating TCRs showed more inhibitory marker expression, indicating feedback regulation. All neoTCRs mediated CD8+ T cell killing while CD8-dependency impacted CD4+ activity with respect to tumor cell killing and cytokine secretion. Tumor cell killing varied by MM cell line, with JJN3 less sensitive than U266B1, though cytokine patterns remained similar.
In conclusion, our in vitro co-culture models confirmed previously detected patterns within our neoTCR-spectrum, also in a myeloma context, adding new information on CD4+ T cells transgenic for these receptors.